Gynecomastia is one of the most misunderstood male health issues in the world. It’s often dismissed as “just fat” or blamed on laziness, yet it can be driven by hormones, medications, genetics, or underlying medical conditions. For many men, it becomes the number one confidence killer in their lives. This guide explains what gynecomastia really is, how to tell if you have it, what causes it, and which treatment options actually work in 2026.
What Is Gynecomastia?
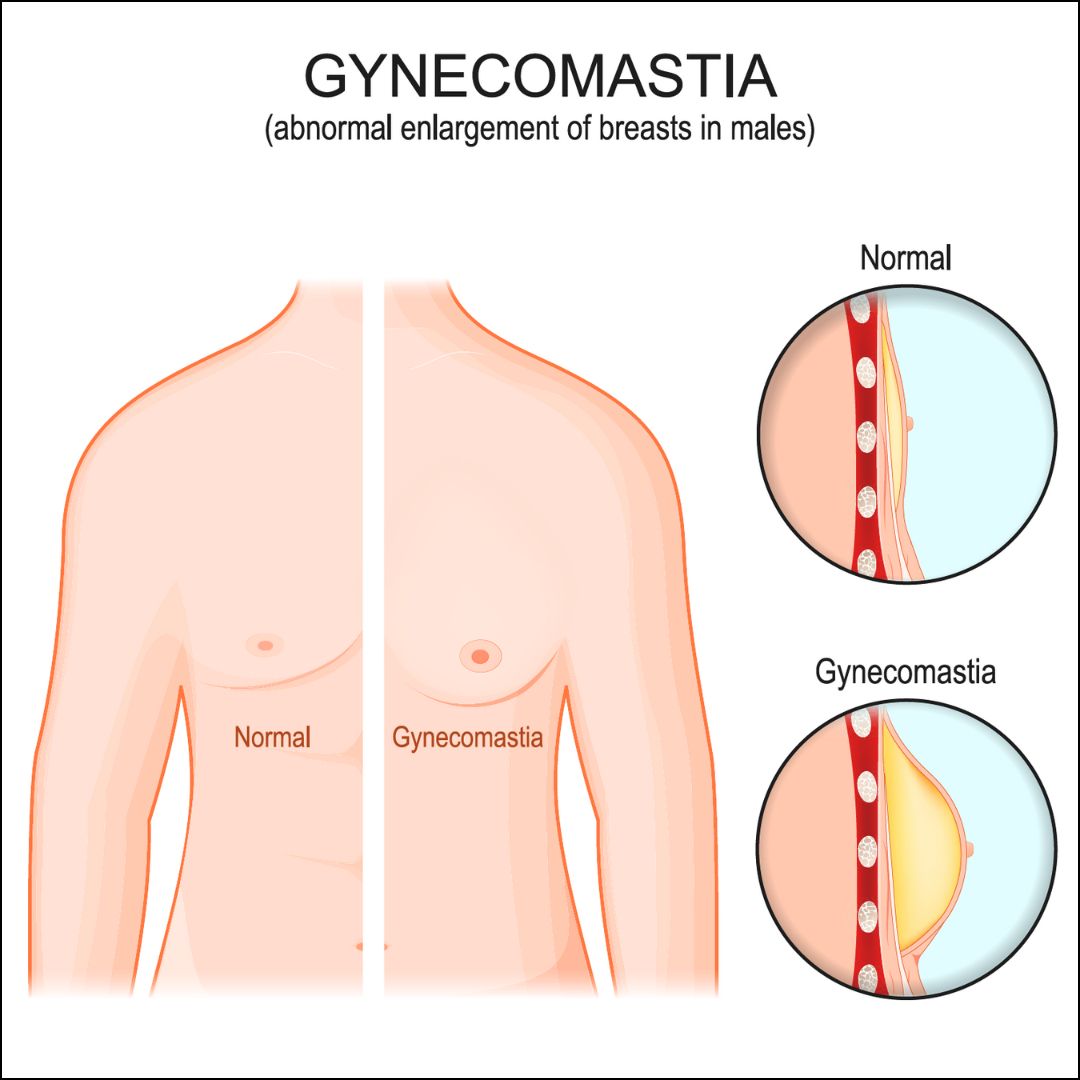
Gynecomastia is the benign enlargement of male breast tissue caused by an increase in glandular tissue, not just fat. It usually appears as:
-
Puffy or enlarged nipples
-
A firm, rubbery lump under the areola
-
One or both sides affected, sometimes asymmetrically
It is different from simple chest fat (sometimes called “pseudogynecomastia”). Chest fat feels soft and spread out, while glandular tissue feels firmer and more localized behind or around the nipple.
True gynecomastia is not cancer, but in rare cases breast cancer can occur in men, so any new or rapidly changing lump should be checked by a doctor.
Types of Gynecomastia
Understanding the type can help you and your doctor decide what to do next.
Pubertal Gynecomastia
This occurs in teenage boys during puberty due to hormone fluctuations. It often:
-
Appears between ages 10–17
-
May feel tender or sore
-
Resolves on its own in many cases within 6–24 months
If breast enlargement persists for several years after puberty, it is more likely to be permanent.
Adult Gynecomastia
This happens in men after puberty and is more likely to be stable or progressive rather than self‑resolving. It can be related to:
-
Hormonal changes with age
-
Medications
-
Medical conditions
-
Lifestyle or substance use
Pseudogynecomastia
This is enlargement of the chest due only to excess fat, not gland. It often improves significantly with fat loss, although some glandular tissue can still coexist.
Common Symptoms and How to Recognize Them
Symptoms can be physical, emotional, or both:
-
Visible enlargement of one or both breasts
-
Puffy or protruding nipples, especially in fitted shirts
-
Firm mass or disk‑like tissue under the nipple
-
Nipple sensitivity or mild pain
-
Embarrassment, avoidance of swimming, fitted clothing, or intimacy
-
Anxiety, low self‑esteem, and social withdrawal
If you notice a hard, fixed lump, nipple discharge (especially bloody), skin dimpling, or changes in the nipple, you should see a doctor promptly to rule out serious conditions.
What Causes Gynecomastia?
Most causes come down to an imbalance between estrogen and testosterone in the body, but there are many possible triggers.
Hormonal Imbalance
Men naturally produce small amounts of estrogen. Gynecomastia can occur when:
-
Estrogen levels are relatively high
-
Testosterone levels are relatively low
-
The breast tissue is unusually sensitive to hormones
This imbalance can be temporary (puberty, acute illness) or long‑term (aging, endocrine disorders).
Medications and Substances
Several common medications and substances can contribute, including but not limited to:
-
Certain antidepressants and antipsychotics
-
Some blood pressure medications
-
Proton pump inhibitors (for reflux)
-
Finasteride and similar drugs used for hair loss or prostate issues
-
Some anabolic steroids and prohormones
-
Alcohol, especially heavy use
-
Some illicit drugs
Never stop prescribed medication without talking to your doctor, but do ask whether a drug could be contributing and whether alternatives exist.
Medical Conditions
Underlying health issues can also play a role:
-
Primary or secondary hypogonadism (low testosterone)
-
Hyperprolactinemia (high prolactin)
-
Thyroid disorders
-
Liver or kidney disease
-
Tumors affecting hormone‑producing glands
Because these can be serious, a proper evaluation is important when gynecomastia appears or worsens unexpectedly.
Lifestyle Factors
Weight gain, poor sleep, chronic stress, and high alcohol intake can indirectly affect hormones and body composition. They may not be the sole cause, but they can worsen a mild tendency.
Gynecomastia vs Chest Fat: How to Tell the Difference
Many men wonder if they have true gynecomastia or just extra fat on the chest.
Signs suggesting more glandular gynecomastia:
-
Firm or rubbery disk of tissue under the nipple
-
Puffy areola that stays protruding even when you flex your chest
-
Little improvement in chest shape despite significant fat loss
Signs suggesting mostly fat:
-
Soft, diffuse tissue without a distinct lump
-
Overall high body fat percentage
-
Chest size decreases clearly with weight loss
Only a qualified clinician can give a definitive assessment, sometimes using ultrasound or other imaging, but understanding this difference helps set expectations.
How Gynecomastia Is Diagnosed
A proper diagnosis usually involves:
-
Medical history
-
When did it start?
-
Is it painful or changing?
-
Medications, supplements, lifestyle habits
-
-
Physical examination
-
Palpation of breast tissue
-
Assessment of testicles, body hair, overall development
-
-
Blood tests (when indicated)
-
Testosterone, estradiol
-
Prolactin
-
LH/FSH (for hypogonadism pattern)
-
Thyroid function
-
Possibly liver and kidney tests
-
-
Imaging (when needed)
-
Ultrasound or mammogram in atypical cases
-
This workup helps distinguish common, benign gynecomastia from rare but important conditions that require different management.
Treatment Options for Gynecomastia in 2026
There is no single solution that suits everyone. Options depend on cause, duration, severity, and personal goals.
1. Watchful Waiting (Mainly for Recent Pubertal Gyno)
For boys in early puberty with recent onset gynecomastia, observation is often appropriate because many cases resolve naturally. Your doctor may:
-
Monitor size and symptoms over time
-
Check for red flags that require further testing
If gynecomastia persists for years or seriously affects mental health, other options may be discussed.
2. Addressing Underlying Causes
When gynecomastia is linked to a specific cause, the first step is to address that:
-
Adjusting or changing a medication (under medical supervision)
-
Treating a thyroid or hormone disorder
-
Reducing alcohol or substance use
-
Managing weight, sleep, and stress
Sometimes, early gynecomastia may improve if the trigger is removed quickly. Long‑standing gland tissue is less likely to regress completely.
3. Medical Therapy (Limited but Sometimes Useful)
Certain medications may be used in selected cases, typically under specialist supervision:
-
Selective estrogen receptor modulators (SERMs) such as tamoxifen or raloxifene have been used in recent or painful gynecomastia.
-
Aromatase inhibitors, which reduce estrogen production, have more limited roles.
-
Prolactin‑lowering drugs may be used if high prolactin is confirmed as the cause.
These drugs are not magic cures and are not appropriate for everyone. They work best when gynecomastia is relatively new and closely related to a hormonal imbalance that can be corrected.
4. Lifestyle and Body Composition Changes
While lifestyle changes don’t remove gland tissue, they can:
-
Reduce overall chest size by lowering body fat
-
Improve chest shape and posture
-
Support hormonal balance and surgical outcomes
A combination of:
-
Strength training (including chest and back)
-
Moderate calorie deficit if overweight
-
Adequate protein intake
-
Good sleep and stress management
can help you feel better and may make any remaining gland less noticeable.
5. Surgery: The Definitive Treatment
Surgery is currently the only way to physically remove glandular breast tissue. It is often considered when:
-
Gynecomastia is long‑standing and stable
-
It causes significant psychological or physical distress
-
Conservative measures have failed
Common techniques include:
-
Liposuction for excess fat
-
Direct gland excision through a small incision
-
Combination procedures for the best contour
-
Nipple/areola reduction or skin tightening in larger cases
Recovery usually involves wearing a compression garment, limiting arm movements for a short period, and avoiding heavy lifting or chest training until cleared by the surgeon.
Emotional and Psychological Impact
Gynecomastia is not “just cosmetic” for many men. It can lead to:
-
Avoidance of social situations involving swimwear or changing rooms
-
Anxiety about intimacy and dating
-
Body image distress and low self‑esteem
-
Depression or social withdrawal
Recognizing this emotional burden is important. Support can come from:
-
Honest conversations with trusted people
-
Online or in‑person support communities
-
Professional mental health support if needed
Working on mindset and self‑acceptance does not mean giving up on treatment; it means reducing unnecessary shame while you decide what is right for you.
When Should You See a Doctor?
You should consult a healthcare professional if you notice:
-
New breast enlargement without clear cause
-
Painful or rapidly growing tissue
-
Hard, irregular, or fixed lumps
-
Nipple discharge or skin/nipple changes
-
Significant impact on your daily life, confidence, or mood
A doctor can help rule out serious causes, explain options, and refer you to specialists (such as endocrinologists or plastic surgeons) if needed.
Frequently Asked Questions About Gynecomastia
Is gynecomastia dangerous?
Most cases are benign and not life‑threatening, but they can signal hormonal or medical issues that should be evaluated.
Can gynecomastia go away on its own?
Pubertal gynecomastia often improves naturally. Long‑standing gynecomastia in adults is less likely to disappear without surgery.
Does losing weight cure gynecomastia?
Weight loss can reduce chest fat and improve appearance, but it cannot remove true gland tissue. In some men, the gland becomes more visible after fat loss.
Can I treat gynecomastia at home?
You can improve lifestyle factors, but you cannot safely self‑medicate with hormones or powerful drugs. Always speak with a doctor before trying any medical therapy.
Is surgery always necessary?
No. Surgery is an option, not an obligation. Some men choose surgery for a permanent solution, while others focus on lifestyle, acceptance, or medical management when appropriate.
Final Thoughts
Gynecomastia is far more common than most men realize, yet it is rarely discussed openly. Understanding the condition—what it is, what causes it, and what can realistically be done—turns confusion and shame into clarity and options. Whether your next step is getting blood tests, talking to a doctor, adjusting lifestyle factors, or researching surgery, the key is this: you are not alone, and you are not broken.
If you’d like, I can now help you turn this guide into a blog post structure for your WordPress site (with a table of contents and SEO‑friendly headings), or adapt it to link naturally to your ebook landing page.
Sources:
1. American Society of Plastic Surgeons: Learn more about gynecomastia surgery
2. Mayo Clinic: Gynecomastia causes and symptoms
3. NIH Study: Medical study on gynecomastia prevalence

